“These participants had experienced brain injury years to decades before, and it was thought that whatever recovery process was possible had already played out, so we were surprised and pleased to see how
much they improved.”
Findings
Discovery
A Window Into the Evolution of Lethal Cancers
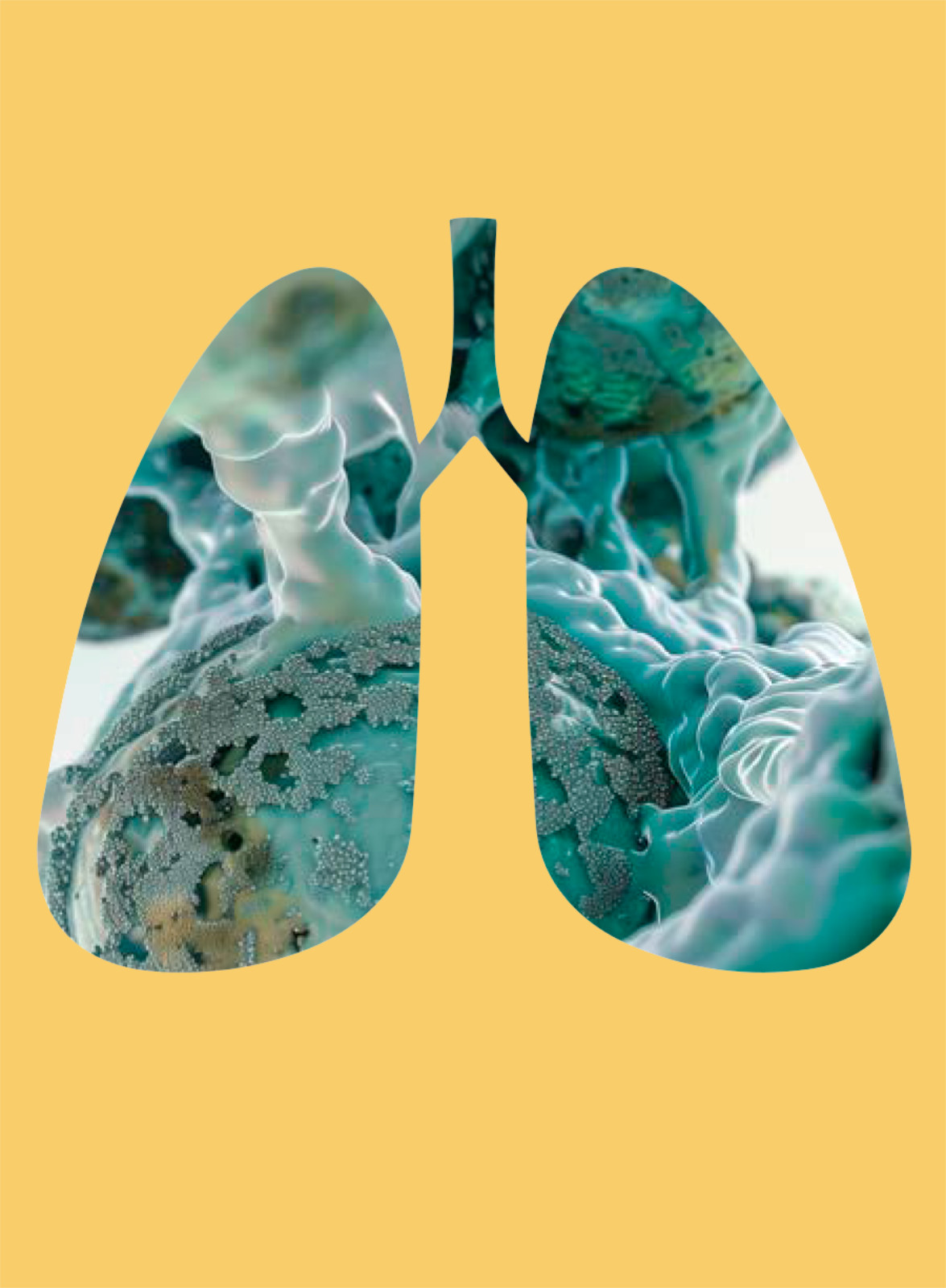
Lung tumors called adenocarcinomas sometimes respond to initially effective treatments by transforming into a much more aggressive small cell lung cancer that spreads rapidly and has few options for treatment. Researchers at Weill Cornell Medicine have developed a preclinical model that illuminates this problematic process, known as histological transformation. The findings advance the understanding of how mutated genes can trigger cancer evolution and suggest targets for more effective treatments.
The researchers, whose results were published in Science, discovered that during the transition from lung adenocarcinoma to small cell lung cancer, the mutated cells appeared to undergo a change in cell identity through an intermediate, stem cell-like state, which facilitated the transformation.
“It is well known that cancer cells continue to evolve, especially to escape the pressure of effective treatments,” says Dr. Harold Varmus, the Lewis Thomas University Professor of Medicine and a member of the Sandra and Edward Meyer Cancer Center. “This study shows how new technologies — including the detection of molecular features of single cancer cells, combined with computer-based analysis of the data — can portray dramatic, complex events in the evolution of lethal cancers, exposing new targets for therapeutic attack.”
Shedding Light on Symptoms of Long COVID

A new study reported that SARS-CoV-2, the virus that causes COVID, can infect dopamine neurons in the brain and trigger senescence — when a cell loses the ability to grow and divide. Further research on this finding may shed light on the neurological symptoms associated with long COVID such as brain fog, lethargy and depression, suggest researchers from Weill Cornell Medicine, Memorial Sloan Kettering Cancer Center and Columbia University Vagelos College of Physicians and Surgeons.
The findings, published in Cell Stem Cell, show that dopamine neurons infected with SARS-CoV-2 stop working and send out chemical signals that cause inflammation. Normally, these neurons produce dopamine, a neurotransmitter that plays a role in feelings of pleasure, motivation, memory, sleep and movement. Damage to these neurons is also connected to Parkinson’s disease.
“This project started out to investigate how various types of cells in different organs respond to SARS-CoV-2 infection. We tested lung cells, heart cells, pancreatic beta cells, but the senescence pathway is only activated in dopamine neurons,” says senior author Dr. Shuibing Chen, director of the Center for Genomic Health, the Kilts Family Professor Surgery and a member of the Hartman Institute for Therapeutic Organ Regeneration. “This was a completely unexpected result.”
1 in 200
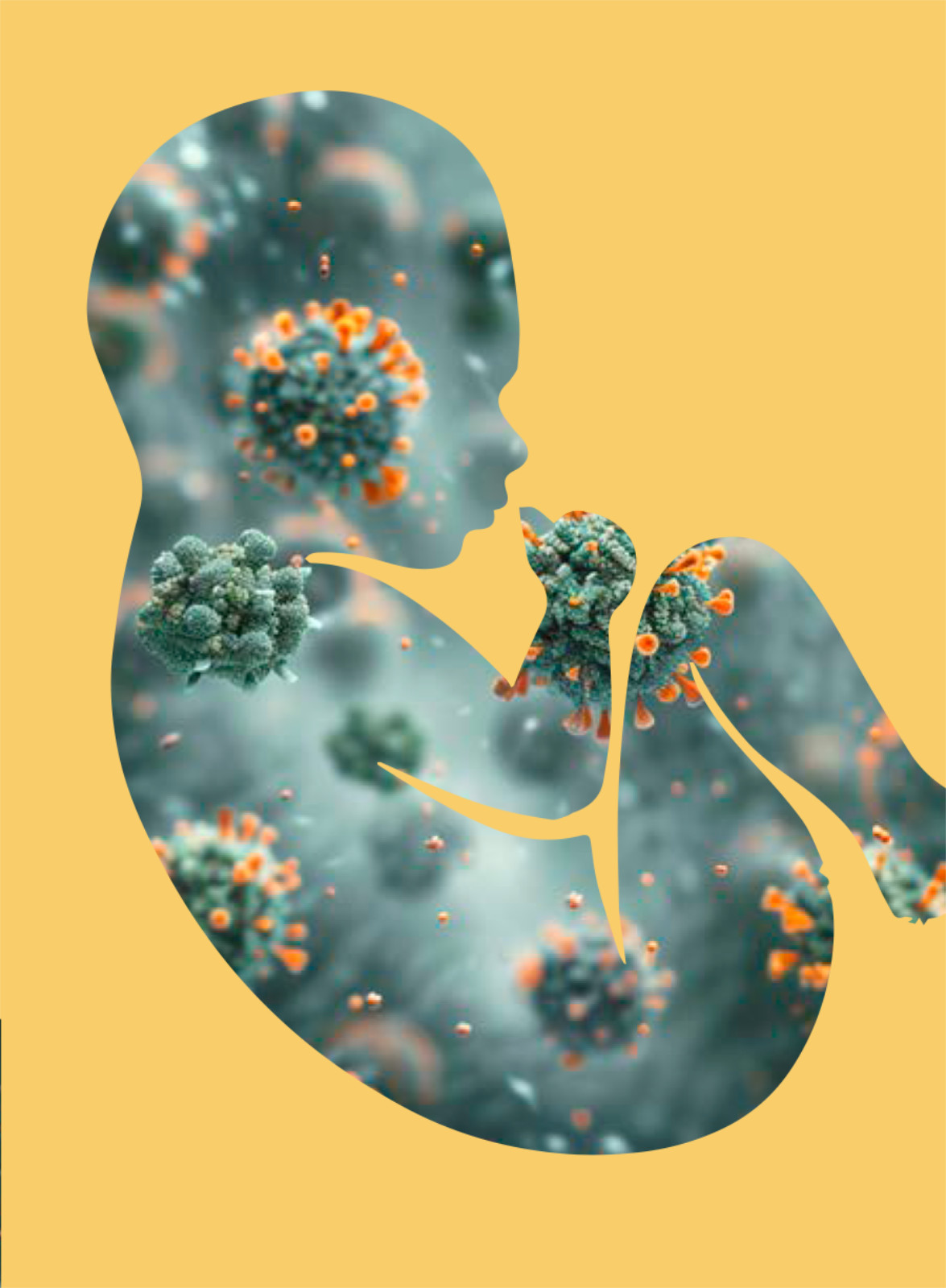
1 in 200: The ratio of newborns worldwide who are infected with human cytomegalovirus (CMV) during their mother’s pregnancy. The virus rarely causes serious illness in healthy adults, but it can cause birth defects and brain damage in newborns infected in utero and deadly infections in immune-compromised adults.
An experimental mRNA vaccine against CMV has elicited some of the most promising immune responses to date of any CMV vaccine candidate, according to a study by Weill Cornell Medicine investigators.
The study, published in the Journal of Infectious Diseases, provided evidence that the new mRNA vaccine candidate, manufactured by Moderna Inc., may protect adults against CMV. Thus, it could potentially prevent women from passing the harmful infection to their babies during pregnancy. Compared with a previous moderately successful vaccine candidate called gB/MF59, the mRNA vaccine elicited responses that were better at preventing the CMV virus from infecting epithelial cells that line the mouth and nose and provide the first line of defense against viral infection. The mRNA vaccine was also more effective at triggering the immune system to destroy CMV-infected cells.
“After more than 50 years of research, we are closer than ever to having a licensed CMV vaccine,” says senior author Dr. Sallie Permar, chair of the Department of Pediatrics and Nancy C. Paduano Professor in Pediatrics. She is also pediatrician-in-chief at NewYork-Presbyterian/Weill Cornell Medical Center and NewYork-Presbyterian Komansky Children’s Hospital.
Genetic Insights Into Weight Gain
A preclinical study by Weill Cornell Medicine investigators shows that a specific human genetic variant of a receptor that stimulates insulin release may help individuals be more resistant to obesity. The researchers discovered that this variant behaves differently in the cell, which may contribute to more efficient metabolism.
The study, posted online in Molecular Metabolism, provides new insight into how human genetic variations affect an individual’s susceptibility to weight gain. The researchers developed mice with a human genetic variant in the glucose-dependent insulinotropic polypeptide (GIP) receptor associated with leaner body mass index (BMI). They found that the mice were better at processing sugar and staying leaner than mice with a different, more common variant of the receptor. The discovery may point to new potential strategies to treat obesity, which affects more than 100 million adults in the United States, according to the Centers for Disease Control and Prevention.
“Our work demonstrates how basic science research can yield important insights about complex biology,” says the study’s senior author Dr. Timothy McGraw, a professor of biochemistry in cardiothoracic surgery and in biochemistry. “These GIP receptors and their behavior at the cellular level profoundly impact metabolism and weight regulation.”
Dr. Nicholas Schiff, the Jerold B. Katz Professor of Neurology and Neuroscience in the Feil Family Brain and Mind Research Institute, co-senior author of a study of five people who had life-altering, seemingly irreversible cognitive deficits following moderate to severe traumatic brain injuries. All showed substantial improvements in their cognition and quality of life after receiving an experimental form of deep brain stimulation (DBS) in a phase 1 clinical trial. The trial, reported in Nature Medicine, was led by investigators at Weill Cornell Medicine, Stanford University, the Cleveland Clinic, Harvard Medical School and the University of Utah.
The findings pave the way for larger clinical trials of the DBS technique and offer hope that cognitive deficits associated with disability following traumatic brain injury may be treatable, even many years after the injury.
Illustrations: Anatomy Blue
Summer 2024 Front to Back
-
Features
Science Over Stigma
By probing the physical cause of obesity, researchers have repudiated harmful misconceptions, leading to new, highly effective medications. -
Features

The Sounds of Science
How insights from ornithology, coupled with advances in AI, could enable doctors to screen for disease using the human voice. -
Features

Bones’ Secret Cells
Research led by Dr. Matthew Greenblatt and his lab is revealing connections between bone stem cells and a surprising array of conditions — including cancer. -
Notable

Expansion in Midtown
A 216,000 square-foot expansion of clinical and research programs at 575 Lexington Ave. will provide state-of-the-art clinical care at the Midtown Manhattan location. -
Notable

A Dramatic Growth in Research
In the decade since the Belfer Research Building’s opening, Weill Cornell Medicine’s sponsored research funding has more than doubled. -
Notable

Dateline
Heart disease presents differently in resource-poor countries like Haiti. Dr. Molly McNairy and colleagues are working to identify underlying causes and prevention. -
Notable

Overheard
Weill Cornell Medicine faculty members are leading the conversation about important health issues across the country and around the world. -
Notable

News Briefs
Notable faculty appointments, honors, awards and more — from around campus and beyond. -
Grand Rounds

Living With Endometriosis: A 12-Year Journey
How the right treatment reduced the pain of endometriosis -
Grand Rounds

Taking Action Against Lung Cancer
Monitoring by Weill Cornell Medicine’s Incidental Lung Nodule Surveillance Program can lead to early cancer detection. -
Grand Rounds
News Briefs
The latest on teaching, learning and patient-centered care. -
Discovery

Gut Check
New evidence shows that a bacterium found in the gut of livestock could be a trigger of multiple sclerosis in humans. -
Discovery
Researchers Chart the Contents of Human Bone Marrow
A new method for mapping the location and spatial features of blood-forming cells within human bone marrow provide a powerful new means to study diseases that affect it. -
Discovery
Findings
The latest advances in faculty research, published in the world’s leading journals. -
Alumni

Profiles
Forging critical connections to move research from the bench to the bedside, our alumni are making an impact. -
Alumni

Notes
What’s new with you? Keep your classmates up to date on all your latest achievements with an Alumni Note. -
Alumni

In Memoriam
Marking the passing of our faculty and alumni. -
Alumni

Moments
Marking celebratory events in the lives of our students, including the White Coat Ceremony and receptions for new students. -
Second Opinion

Equal Risk
Does race have a role in calculations of health risks? -
Exchange

Health Equity
Two faculty members discuss the importance of community-engaged research in their work to help combat cancer disparities fueled by persistent poverty. -
Muse

Finding Strength in Art
Surin Lee is a Weill Cornell Medicine-Qatar medical student, Class of 2026, and a visual artist. -
Spotlight

Partners in Solving Surgical Challenges
Dr. Darren Orbach (M.D. ’98, Ph.D.) and Dr. Peter Weinstock (M.D. ’98, Ph.D.) are pioneering the use of practice simulations to ensure successful complex surgeries.